John Whyte, MD, Chief Medical Officer at WebMD said, “We have been seeing a high mortality for patients once they are put on a ventilator. Part of the challenge is that we don’t always have enough data early-on in an epidemic. That’s why it is important to talk to physicians on the front-lines and hear about what they are seeing. This creates more discussion and debate in the clinical and scientific community to help us determine the most effective treatment strategies.”
The ICU doctor in the video below (which has gone viral) from New York suggests that we are treating the wrong disease with the wrong measures. WebMD published, “As doctors treat more patients who are severely ill from COVID-19, they’re noticing differences in how their lungs are damaged. Some patients coming to the hospital have very low oxygen levels in their blood, but you wouldn’t necessarily know it from talking to them. They don’t seem starved of oxygen. They may be a little confused. But they aren’t struggling to breathe.”
“When doctors take pictures of their lungs — either with a CT scanner or an X-ray machine — those also look fairly healthy. The lungs may have a few areas of cloudiness and crazing, indicating spots of damage from their infection, but most of the lung is black, indicating that it is filled with air.”
It was “as if tens of thousands of my fellow New Yorkers are stuck on a plane at 30,000 feet and the cabin pressure is slowly being let out. These patients are slowly being starved of oxygen,” said Cameron Kyle-Sidell, MD, an emergency room and critical care doctor at Maimonides Medical Center in Brooklyn.
“A whole bunch of these patients really have low oxygen, but their lungs don’t look all that bad,” says Todd Bull, MD, director for the Center of Lungs and Breathing at the University of Colorado School of Medicine, in Aurora.
“Doctors in Italy have noticed the same thing. And in some cases, that might mean patients need to be treated a little differently to ensure the best outcome,” writes WebMD.
In an editorial in the journal Intensive Care Medicine, Luciano Gattinoni, MD, a guest professor of anesthesia and intensive care at the University of Gottingen in Germany, and one of the world’s experts in mechanical ventilation, says more than half the patients he and his colleagues have treated in Northern Italy have had this unusual symptom. They seem to be able to breathe just fine, but their oxygen is very low.
Tissue hypoxia, as a result of cardiopulmonary dysfunction or reduced oxygen-carrying capacity, is a frequently encountered clinical problem.
“The past 48 hours or so have seen a huge revelation: COVID-19 causes prolonged and progressive hypoxia (starving your body of oxygen) by binding to the heme groups in hemoglobin in your red blood cells. People are simply desaturating (losing o2 in their blood), and that’s what eventually leads to organ failures that kill them, not any form of ARDS or pneumonia. All the damage to the lungs you see in CT scans are from the release of oxidative iron from the hemes, this overwhelms the natural defenses against pulmonary oxidative stress and causes that nice, always-bilateral ground glass opacity in the lungs. Patients returning for re-hospitalization days or weeks after recovery suffering from apparent delayed post-hypoxic leukoencephalopathy strengthen the notion COVID-19 patients are suffering from hypoxia despite no signs of respiratory ‘tire out’ or fatigue.”
Dr. Isaac Solaimanzadeh, practitioner of Internal Medicine at the Interfaith Medical Center in Brooklyn, is also supporting what Dr. Kyle-Sidell is saying in the video about coronavirus being something more like high altitude high altitude pulmonary edema than a viral driven pneumonia. He stated:
“While anti-viral approaches and vaccines are being considered immediate countermeasures are unavailable. Both COVID-19 and HAPE exhibit a decreased ratio of arterial oxygen partial pressure to fractional inspired oxygen with concomitant hypoxia and tachypnea. There also appears to be a tendency for low carbon dioxide levels in both as well.”
Under clinical conditions, low oxygen and low carbon dioxide generally occur together. Therapeutic increase of carbon dioxide, by inhalation of this gas diluted in air, is often an effective means of improving the oxygenation of the blood and tissues. If the level of carbon dioxide in the blood is lower than normal, then this leads to difficulties in releasing oxygen from haemoglobin.
There are many reasons for hypoxia starting with severe mineral deficiencies and over-breathing, which lowers both oxygen delivery and carbon dioxide in the blood.
Abnormal magnesium deprived red blood cells lack
flexibility that allow them to enter tiny capillaries.
Recognition of inadequate oxygen delivery to the cells can be difficult in the early stages because the clinical features are often non-specific. Progressive metabolic acidosis, hyperlactataemia, and falling mixed venous oxygen saturation (SvO2), as well as organ specific features are not noticed usually until its too late and serious disease sets in.
Iodine and Oxygen
Iodine-carrying thyroid hormones are essential for oxygen-based metabolism.
First increases of iodine and thyroid hormones increase red blood
cell mass and increase the oxygen disassociation from hemoglobin.
Thyroid hormones have a significant influence on erythropoiesis, which is the process that produces red blood cells (erythrocytes). The most common thyroid dysfunctions, hypothyroidism and hyperthyroidism affect blood cells and cause anemia with different severity. Thyroid dysfunction and iodine deficiency induces other effects on blood cells such as erythrocytosis, leukopenia, thrombocytopenia, and in rare cases causes’ pancytopenia. Iodine also alters RBC indices include MCV, MCH, MCHC and RDW.
Thyroid hormone increases oxygen consumption, increase mitochondrial size, number and key mitochondrial enzymes. Meaning iodine increases plasma membrane Na-K ATPase activity, increases futile thermogenic energy cycles and decreases superoxide dismutase activity.
A deficiency of red blood cells, or anemia, limits the
oxygen-carrying capacity of the blood, potentially
leading to reduced total oxygen content in the bloodstream.
5 G and Oxygen
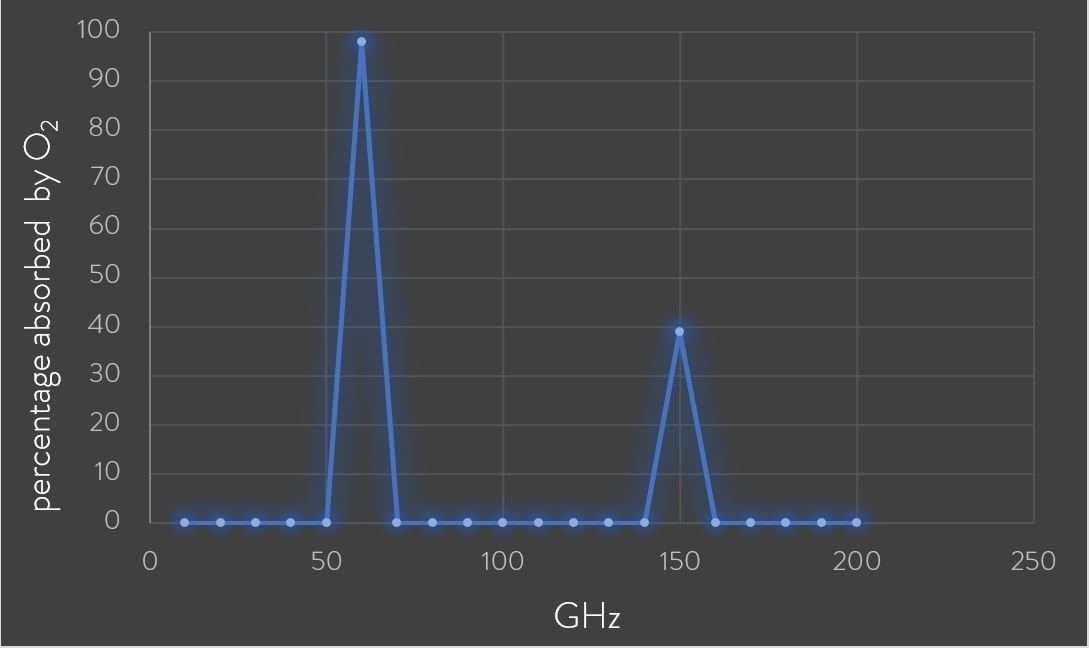
The 60GHz Oxygen Absorption Band
The promotional materials from Telecom companies brag that 5G messes with oxygen molecules. When you hit oxygen molecules with 60 GHz millimeter wave emissions it affects the orbital properties of the electrons of the oxygen molecules. The 60 GHz range is known as the Oxygen Absorption Band. At 60GHz, 98% of electromagnetic energy is absorbed by O2. When 5G reaches the frequency band of 60 GHz, the ability for a person’s blood hemoglobin to bind with oxygen is hindered and this might explain, in part, why people in Wuhan just fell down dead in the streets, which is not a normal thing we see with viral infections.
Poor immune function and ill health combined with environmental stress such as heightened EMF exposure might create a perfect storm where the virus has an easy way to get into the body and can reproduce faster. We all are aware that EMF is not the healthiest thing in the world and a case has been made that EMFs might make us more susceptible or sensitive to viral illnesses. Many of the areas hardest hit by COVID-19 have recently implemented 5G, which might render residents more prone to serious infection by lowering their immune function
Magnesium and Oxygen
Mineral deficiencies help create hypoxic conditions, especially when they are needed to neutralized chemical and heavy metal toxins. Also, certain minerals are needed by the red blood cells to do their jobs efficiently. Magnesium deficient diet leads to significant decreases in the concentration of red blood cells (RBC), hemoglobin and eventually a decrease in whole blood Fe.
We find many ways in which magnesium deficiency leads to problems with oxygen transport and utilization. Iron of course is at the heart of hemoglobin so any deficiencies there are telling. And because many pharmaceutical drugs drive down magnesium levels they must be considered as major causes of lowered oxygen delivery to the cells.
The mechanism whereby red cells maintain their biconcave shape has been a subject of numerous studies. One of the critical factors for the maintenance of biconcave shape is the level of red cell adenosine triphosphate (ATP) levels. The interaction of calcium, magnesium and ATP with membrane structural proteins exerts a significant role in the control of shape of human red blood cells. Magnesium enhances the binding of oxygen to haem proteins.
Chloroquine
How does chloroquine work? Same way as it does for malaria. You see, malaria is this little parasite that enters the red blood cells and starts eating hemoglobin as its food source. The reason chloroquine works for malaria is the same reason it works for COVID-19 — while not fully understood, it is suspected to bind to DNA and interfere with the ability to work magic on hemoglobin. The same mechanism that stops malaria from getting its hands on hemoglobin and gobbling it up seems to do the same to COVID-19.
A Lack of Sunlight
UV is needed to utilize oxygen in the blood. UV increases nitric oxide and the relaxation of blood vessels. UV increase free endothelial NOS/eNOS (in vessels/capillaries) and total neuronal NOS/nNOS (in neurons) and increases nitric oxide through other means (R), which allows oxygen to diffuse into tissues better. UV also relaxes your blood vessels by mechanisms that might be independent of NO (R).
Heavy Metals and Oxygen
The structure of hemoglobin is easily compromised by heavy metals like mercury. All carcinogens impair respiration directly or indirectly by deranging capillary circulation, a statement that is proven by the fact that no cancer cell exists without exhibiting impaired respiration.
“Tumors cannot grow if the oxygen levels are normal, and oxygen levels are controlled by voltage,” says Dr. Jerry Tennant. He could have said oxygen levels are controlled by pH or oxygen levels control voltage because if there is too little oxygen then the mitochondria cannot create enough ATP to keep cellular energy high.
Conclusion
Speaking from the perspective of intensive care, Dr. R M Leach and Dr. D F Treacher say, “Prevention, early identification, and correction of tissue hypoxia are therefore necessary skills in managing the critically ill patient and this requires an understanding of oxygen transport, delivery, and consumption.”
Red blood cells have been reported to shrink and become stiffer under hypoxic conditions leading to a downward spiral in oxygen transport and delivery. So, “Early detection and correction of tissue hypoxia is essential if progressive organ dysfunction and death are to be avoided. However, hypoxia in individual tissues or organs caused by disordered regional distribution of oxygen delivery or disruption of the processes of cellular oxygen uptake and utilization cannot be identified from global measurements. Regional oxygen transport and cellular utilisation have an important role in maintaining tissue function. When tissue hypoxia is recognised, treatment must be aimed at the primary cause,” write Leach and Treacher.
Biologist Dr. Ray Peat tells us that, “Breathing pure oxygen lowers the oxygen content of tissues; breathing rarefied air, or air with carbon dioxide, oxygenates and energizes the tissues; if this seems upside down, it’s because medical physiology has been taught upside down. And respiratory physiology holds the key to the special functions of all the organs, and too many of their basic pathological changes.”
Dr.Sircus is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
Subscribe now




comments