
MAGNESIUM CHLORIDE INJECTION
200mg/mL (20% w/v), 2.951 mOsm/mL, 50mL Multi-Dose Vial.
The only real challenge with magnesium is getting it into your body, because most products are poorly absorbed and cause diarrhea. But once I solved this problem and was able to increase my magnesium intake, my pain quickly eased and my disorder gradually faded.– Dr. Jay S. Cohen
The use of high oral doses of magnesium has typically been precluded because of magnesium’s tendency to provoke diarrhea in many patients when administered orally. For example, in one study a dosage of 250 mg two times daily of magnesium administered orally produced adverse intestinal effects in 45.7% of subjects. For many years oral dosing was without question the administration route of choice for most doctors and healthcare practitioners. Intravenous drug administration requires that the patient be in a hospital or clinic though when the condition being treated is chronic, this is impractical and expensive.
Administration with magnesium at pharmacologic doses is crucial to treating chronic conditions that are arising from common and persistent magnesium deficiencies. However oral dosing at pharmacologic levels has heretofore been ineffective due to the inability of patients to tolerate such a regimen. This problem is now academic since the advent of transdermal dosing, which has arisen in popularity only in the last three years.
There have been several doctors who have been able to optimize oral intake through several daily administrations, totaling approximately 2-12 times the RDA for magnesium (600 mg to 5 gm elemental magnesium). Dr. Jay S. Cohen, a nationally recognized expert on medications and side effects and the author of The Magnesium Solution for High Blood Pressure submitted a patent with this gradually increasing oral protocol. These higher levels are achieved through increasing daily dosage amounts gradually in response to patient tolerance and using a more well-tolerated form of magnesium preferably a magnesium chloride solution. Total magnesium intake is divided over several doses per day and taken with copious amounts of water.
Orally administered magnesium dosage levels can be increased gradually over time from about 250 to 500 mg elemental magnesium/day to between about 600 mg and about 5000 mg/day elemental magnesium, wherein each orally administered daily dosage amount is divided into smaller doses and orally administered several times per day. The orally administered daily dosage amount is gradually increased over time and in association with patient’s increased tolerance to the increased dosage, and the administered magnesium is in a solid form or a solution; and maintaining a well-tolerated high-level dosage of orally administered magnesium until cell levels rise and signs and symptoms recede. One retired doctor with diabetic neuropathy was able to tolerate up to 20 grams a day in this way and was able to control his neuropathy.
The preferred magnesium treatment uses a magnesium compound in solution, such as intravenous grade MgSO 4 or MgCl in water or dextrose solution. Other magnesium compounds effective in the present invention include magnesium acetate, magnesium carbonate, magnesium citrate, magnesium gluconate, magnesium glycinate, magnesium hydroxide, magnesium maleate, magnesium orolate, maxnesium oxide, magnesium succinate, magnesium taurate and chelated forms of magnesium with proteins or amino acids.
If you’re ever rushed to the hospital with a heart attack, intravenous magnesium could save your life. In a 1995 study, researchers found that the in-hospital death rate of those receiving IV magnesium was one-fourth that of those who received standard treatment alone. In 2003, a follow-up study of these same patients revealed an enduring effect of magnesium treatment. Nearly twice as many patients in the standard treatment group had died compared to those who received magnesium, and there were considerably more cases of heart failure and impaired heart function in the placebo group.
In addition to increasing survival after heart attack, IV magnesium also smoothes out arrhythmias and improves outcomes in patients undergoing angioplasty with stent placement. It is also beneficial for acute asthma attacks, often working to relax airway spasms when drugs do not. Magnesium supplementation is crucial for diabetics, too, because it improves insulin sensitivity, helps blood sugar control, and reduces risk of retinopathy.
Therapy with magnesium is rapid acting, has a safe toxic-therapeutic ratio and is easy to administer and titrate.[1] Magnesium is economical, widely available and has a long established safety and tolerability profile in myocardial infarction. Magnesium chloride has the advantage of being administered intravenously, intramuscularly, and orally as well as vaporized through a nebulizer, and as a lotion transdermally. In anesthesia and intensive care, the preferred administration route is IV.
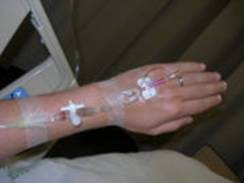
Magnesium ions cross the intact blood-brain barrier efficaciously so that intravenous magnesium significantly raises cerebrospinal fluid and brain extracellular fluid magnesium levels quickly.
In the 90’s cardiovascular biologist Dr. Burton M. Altura of the State University of New York Health Science Center at Brooklyn witnessed a therapeutic benefit of magnesium in acute symptoms, such as headache pain. Altura administered a solution containing 1 gram of magnesium sulfate intravenously to 40 patients who visited a headache clinic in the throes of moderate to severe pain. They treated not only migraine sufferers but also persons with cluster headaches and chronic daily headaches.
Within 15 minutes, 32 of the men and women—80 percent—experienced relief. Though the headache may not have vanished, the pain lessened by at least 50 percent. In 18 of these individuals, the pain relief lasted at least 24 hours. Blood tests before treatment confirmed that all but four in this latter group had ionized magnesium concentrations that were lower than the average in a related group of pain free individuals. “All nine patients with cluster headaches had their acute headache aborted by magnesium therapy.” Migraine sufferers who responded to the treatment experienced a complete alleviation of their current symptoms, including sensitivity to lights and sound. Subsequent studies of additional migraine patients have confirmed a common pattern, Altura says. “Those patients where ionized magnesium in the brain or blood is low will respond to intravenous magnesium very quickly and dramatically.“
The following chapter introduces transdermal medicine, an extraordinary method of magnesium application that has not been studied by allopathic medical science. This chapter focuses on western medicine’s experience with intravenous magnesium infusions and injections. Doctors need to learn though, about and use the wide spectrum of administration routes to harness the full medicinal power of magnesium.
Heart palpitations, “flutters” or racing heart, otherwise called arrhythmias, usually clear up quite dramatically on 500 milligrams of magnesium citrate (or aspartate) once or twice daily or faster if given intravenously.– Dr. H. Ray Evers
Magnesium has minimal side effects in usual therapeutic doses and has a large therapeutic index. The timing and doses of magnesium are critical especially in cases of stroke or heart failure. The Fast-Mag (Field Administration of Stroke Therapy – Magnesium (FAST-MAG) trials are being carried out in Los Angeles to show the beneficial effects of early magnesium administration by paramedics when stroke first occurs. Each year in the US, over 750,000 Americans suffer a symptomatic stroke.

Magnesium chloride is first aid for the heart.
More than 4 out of 5 strokes are due to ischemic infarction.
The FAST-MAG trial was designed to address the crucial factor of delayed time to treatment, which has hindered past human clinical trials of neuroprotective drugs. Animal studies suggest the duration of the therapeutic window is very brief, generally less than 2-3 hours. Most animal studies of neuroprotective agents initiate therapy within 1-60 minutes after ischemia onset. Because magnesium medicine is poorly understood by western medicine it is rarely used early enough or often enough to benefit from its full potential to save lives or reduce suffering among cardiac or stroke patients.
Cardiac arrhythmias and coronary artery vasospasm can be caused by magnesium deficiency and intravenous magnesium reduces the risk of arrhythmia and death immediately after acute myocardial infarction.[2]
A study published in The Lancet reported the effects of a double-blind, randomized, placebo-controlled study in 2,316 patients with suspected myocardial infarction. The dose of magnesium was high (about 8.7 grams given intravenously over a 24 hour period), but the results were remarkable: magnesium reduced cardiovascular mortality by 25 percent. Teo and colleagues, in an analysis of seven clinical studies, concluded that magnesium (in doses of 5-10 grams by intravenous infusion) reduced the odds of death by an astounding 55%. Two forms of Mg are available, namely Mg chloride and sulfate for infusion. Ten millilitres of a 10% Mg chloride (MgCl2) solution provide 1 g of Mg salts (= 118 mg Mg = 9 mEq = 4.5 mmol), and 10 mL of a 10% Mg sulfate (MgSO4) solution provide 1 g of Mg salts (= 98 mg Mg = 8.12 mEq = 4.06 mmol).
Although intravenous magnesium is the drug of choice at the onset of a heart attack, it is not mentioned in the section on arrhythmias in the 1989 “Compendium of Drug Therapy.”– Dr. H. Ray Evers

Dr. Sarah Myhill has been using I.V. magnesium in her general practice for over 15 years for both acute and chronic problems. She uses it for all patients with acute chest pain (unless the blood pressure is very low), acute heart failure, pulmonary embolus and acute asthma. Myhill says, “It is a potent vasodilator – i.e. it opens up all the blood vessels. Indeed patients can feel their blood vessels dilating as I give them the magnesium – they warm up all over! This has the immediate effect of reducing the work of the heart and opening up the co-lateral circulation of the heart. Most of the patients with acute heart attacks have their pain completely relieved by I.V. magnesium.”
“I then give them morphine as well (standard treatment) to relax them and take the stress out of the situation. (Anyone having a heart attack will naturally be in fear of their lives – the panic and adrenaline this creates puts even more stress on the heart). It is anti-dysrythmic – most patients who die from a heart attack do so because the pace maker is disturbed and the heart goes off into an abnormal beat. Magnesium is highly protective against this. It inhibits blood clotting and so reduces the likelihood of further clogging of the blocked artery.”
Myhill continues, “It protects against “stunning” or reperfusion injury. After an acute heart attack, the muscle dies and becomes the infarcted area. With recovery there may be renewed blood supply to the damaged area. The damaged heart muscle may not be able to cope with the renewed oxygen supply and suffer stunning – an acute loss of its contractile ability. This may explain deaths which occur a few hours or days after the initial infarction. In the many patients where I have injected magnesium prior to admission to the hospital, I have never had a patient die subsequently. Indeed I can relieve pain quickly and send them on greatly reassured that all will be well. This technique was taught to me by Dr. Sam Browne who documented his cases (Journal of Nutritional Medicine 1994, 169-177).”
Magnesium has been used safely by doctors for over 60 years. Magnesium’s powerful vasodilator action immediately became apparent with its action increasing in potency with increased initial blood concentrations. After magnesium infusions there is a significant increase in cardiac output, and the cardiac index is maintained at a higher level than that of control groups during the induction of anesthesia and endotracheal intubation.[3]
The common procedure of invasive cardiac intervention and intravenous magnesium administration before reperfusion should without question become the gold standard in treatment of acute myocardial infarction.[4] Two meta-analyses studied the impact of magnesium treatment on reduction of the death rate and rhythm disorders in the acute phase of myocardial infarction before initiation of reperfusion treatments. Both reports found a 54% reduction of the death rate, and one noted a decreased incidence (49% less) of ventricular fibrillation or tachycardia in the population treated by magnesium.[5] The most important action of MgSO4 in AMI is to open up collateral circulation and relieve ischaemia thus reducing infarct size and mortality rates.[6]
Magnesium is far down the pre-hospital protocol though and is not commonly used except in the case of early-recognized Torsades de Pointes, which is a special form of polymorphic ventricular tachycardia. Lidocaine is usually the first medication given someone suspected of heart attack, and its benefit is most likely limited to ventricular tachycardia caused by cardiac ischemia.[7]
During myocardial infarction, serum magnesium drops. Heart muscle cells have a high concentration of total magnesium (11–17 mmol•L-1 of intracellular water).2, 6 Hypomagnesemia, defined as a plasma concentration below 0.7 mmol•L-1, is considered severe when under 0.5 mmol•L-1. This condition is most often associated with a true depletion of magnesium in the organism, although a magnesium deficit can exist even when serum magnesium is normal because the serum levels are maintained within strict limits even as cellular levels drop. Measurement of the urinary excretion of magneisum and a loading test can help establish a diagnosis,37 though magnesium deficit can be universally assumed in most critically ill patients. Incidences of deficit are found to be much higher in patients sampled in surgical and medical intensive care units. For patients with variant angina, 24-hour magnesium retention after intravenous magnesium loading was 60%, while it was only 36% in control subjects.
In the emergency treatment of tetanus magnesium infused at doses providing serum concentrations of 2 to 4 mmol•L-1 allowed good control of spasms and muscle rigidity. Intubation and ventilation were only required for 43% of patients, and the overall death rate was 12%.[8]
Studies looking at the beneficial effects of magnesium administration to critically ill patients in the ICU with a wide range of diagnoses showed that after infusion of 5 gm of magnesium in D5W over 6 hours:
1. Heart rate came down within an average of 45 min, rhythm improved from irregular to regular and to good volume.
2. Urine output increased from almost oliguria to 30–40 ml/hour. Creatinine reduced or did not rise any further.
3. Pulmonary edema resolved in 24 hours.
4. Lactic acidosis disappeared within 4–5 hours.[9]
A total of 126 patients with proven angina have been treated with IV MgSO4 and 116 have either been completely relieved of pain or markedly improved.[10] Most patients were given six IV injections of MgSO4 with a total dose of between 24 and 48 mmol of Mg. If the patient is quite happy, the dose is often increased to 8 mmol given on a further five occasions either daily or weekly as is found convenient. In AMI, I give 7 mmol MgSO4 with 5000 units of heparin in about 15 seconds after an initial 1 mmol has been given more slowly. Then, MgSO4 (8 mmol) is given daily for 2-3 days, or for longer if chest pain recurs. A further course of three doses of 8 mmol is given after 2-3 weeks. In AMI, the dose is reduced to 1 mmol or less, repeated at 15-min intervals, if the blood pressure has fallen unduly.
In some patients with AMI, IV MgSO4 can produce a fall in blood pressure which, if not excessive, may be more beneficial than harmful. In severe cardiogenic shock, the dosage of Mg has been reduced from 8 mmol to 1 mmol or even 0.20 mmol repeated at 15-min intervals with blood pressure monitoring until 4 mmol have been given.[11] Singh has reported dramatic improvement in severe shock using an IV vasodilator.[12]
The treatment to fully replete magnesium levels becomes even more urgent when pharmaceutical medications are used because most drugs drive down magnesium levels further.[13] Magnesium deficiency is routinely made worse by the very drugs meant to help heart problems. “Few doctors know that diuretics help flush magnesium as well as potassium from the body. The resulting magnesium deficiency hinders potassium use by the cells. “Magnesium deficiency keeps people from replenishing potassium,” says hypertension expert Dr. Chris Mende.
Special Note: Vasodilators and nitric oxide supplements are products that help your blood vessels to dilate (open up). These are generally used to help address medical issues like coronary artery disease (condition of the heart that makes blood vessels narrow) and hypertension. It helps to know the best way to increase nitric oxide levels.
[1] Crippa G, Sverzellati E, Giorgi-Pierfranceschi M, et al. Magnesium and cardiovascular drugs: interactions and therapeutic role. Ann Ital Med Int. 1999 Jan; 14(1):40-5.
[2] Eisenberg MJ, Magnesium deficiency and sudden death (editorial), AM Heart J 1992 Aug; 124(2):544-9
[3] The Effect of Magnesium Sulphate on Hemodynamics and Its Efficacy in Attenuating the Response to Endotracheal Intubation in Patients with Coronary Artery Disease G. D. Puri, MD, PhD*, K. S. Marudhachalam, MD, DA, DNB*, Pramila Chari, MD, FAMS, MAMS, DA?, and R. K. Suri, MS, FAMst Departments of *Anaesthesia and Intensive Care and tcardiothoracic and Vascular Surgery, Postgraduate Institute of Medical Education & Research, Chandigarh, India http://www.anesthesia-analgesia.org/cgi/reprint/87/4/808.pdf
[4] Smetana, R. Wink, K. Magnesium, acute myocardial infarction and reperfusion injury. Medicine and Konrad Wink, University Clinic Internal Medicine IV (Vienna, Austria). Clin Calcium. 2005 Feb;15(2):261-4
[6] The Case for Intravenous Magnesium Treatment of Arterial Disease in General Practice: Review of 34 Years of Experience S. E. BROWNE MB BCH
[7]http://209.85.141.104/search?q=cache:8q205pwjZDMJ:www.bernco.gov/upload/images/fire_rescue/
0405_Protocol_Changes.pdf+emt+protocol+for+magnesium+use&hl=en&ct=clnk&cd=1&gl=us
[8] Attygalle D, Rodrigo N. Magnesium as first line therapy in the management of tetanus: a prospective study of 40 patients. Anaesthesia 2002; 57: 778–817.[Medline]
[9] Magnesium in the intensive care unit; from 21st International Symposium on Intensive Care and Emergency Medicine Brussels, Belgium. 20–23 March 2001; Critical Care 2001, 5(Suppl 1):P207 http://ccforum.com/content/5/S1/P207
[11] Browne SE. Intravenous magnesium sulphate in arterial disease. The Practitioner 1969: 202: 562-4.
[12] Singh SP. Use of vasodilator drug in shock (letter). Br Med J 1966; 2: 765.
[13] Most therapeutic drugs (diuretics, chemotherapeutics, immunosuppressive agents, antibiotics) cause hypomagnesemia due to increased urinary loss. It is concluded that most of the clinical situations studied show hypomagnesemia due to renal loss, with exception of renal disease.
Dr.Sircus is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
Subscribe now



comments